 go back
go back
Hives (Urticaria)
Hives, also known as Urticaria, occur as a sudden outbreak of bumps and welts on the skin. These bumps and welts are typically pale red in color and are sometimes accompanied by swelling known as angioedema.
Make An AppointmentHives are a very common skin condition, estimated to occur in 1 in 5 people at some point in their lives.
*American College of Allergy, Asthma & Immunology

What are hives?
Hives can be as small as a dime or much larger. Hives can appear anywhere on the body, including the lips, tongue, throat, and ears, and often resolve on their own.
Hives aren’t contagious. They’re triggered by an immune response in the body and the release of histamines. You won’t develop hives on your skin if you touch the affected skin of another person.
Types of hives
There are both acute and chronic versions of hives. Acute urticaria lasts less than six weeks, while chronic urticaria lasts longer than six weeks. In some cases, hives can be caused by direct touch with cold, heat, sweat, or pressure. This kind of urticaria is called “physical urticaria.”
Chronic hives or chronic urticaria
Chronic hives don’t have a common cause, and it’s hard to figure out what makes them happen.
Both chronic and acute hives can be caused by the same things. They can also be caused by conditions that affect the immune system, long-term infections, or hormonal problems.
Acute hives or acute urticaria
With acute hives or acute urticaria, it’s typically easy to identify a trigger.
Triggers commonly include food, medicine, insect bites, or even latex.
What causes hives?
Hives can be caused by any number of triggers, including allergic reactions, drugs, certain chemicals in foods, or environmental triggers. Oftentimes, it can be difficult to attribute a single cause to an outbreak of hives.
When the body encounters one of these triggers, it releases a chemical known as histamine. This histamine then triggers small leaks of blood plasma out of very small blood vessels in the skin, resulting in both hives and, on occasion, angioedema.
01
Medication
Medications can also trigger hives. NSAIDs, like aspirin and ibuprofen, can cause hives, as well as some high blood pressure medications, including ACE inhibitors. Common painkillers such as codeine have also been associated with the development of hives.
02
Viral
Finally, it may be a virus that causes hives in some patients. Viruses that can trigger hives include the common cold, urinary tract infections, strep throat, mono, and hepatitis. Causes of hives in adults can vary from causes in children, who are often more affected by viral triggers.
Most common triggers for hives
Common triggers for hives include:
- Some food (especially peanuts, eggs, nuts and shellfish)
- Medications, such as antibiotics (especially penicillin and sulfa), aspirin and ibuprofen
- Insect stings or bites
- Physical stimuli, such as pressure, cold, heat, exercise or sun exposure
- Latex
- Blood transfusions
- Bacterial infections, including urinary tract infections and strep throat
- Viral infections, including the common cold, infectious mononucleosis and hepatitis
- Pet dander
- Select plants
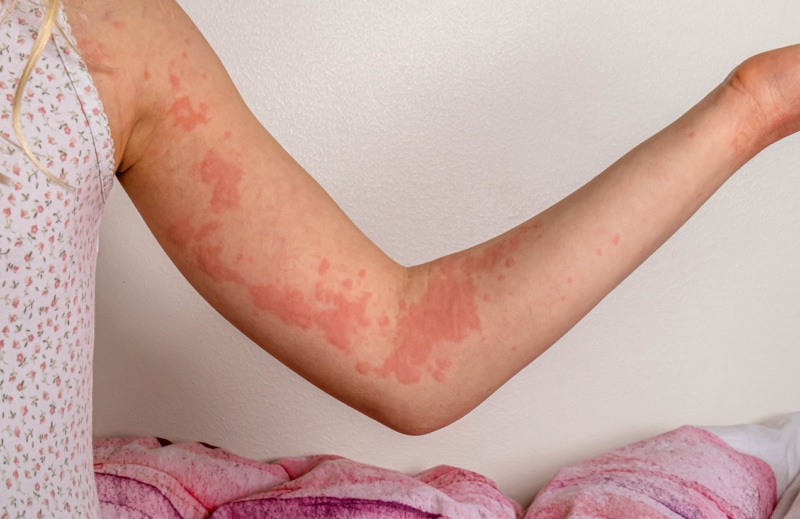
What do hives look like?
Hives can look like small red bumps or larger patches of raised skin. They can be itchy. They can also seem to move from one part of the body to the other.
Hives generally have a distinct appearance with a central, white or lighter-colored area surrounded by a red border.
These skin eruptions may come and go rapidly, appearing on one part of your body and then vanishing, only to reappear elsewhere. It’s also important to note that hives can merge together, forming larger areas known as plaques.
Angioedema without hives
Angioedema, swelling of the skin and fatty tissue, may occur with hives. It can also occur by itself and usually shows up in the face, throat, hands and feet.
Angioedema that occurs without hives can be due to: Aspirin or anti-inflammatory drugs, ACE inhibitors, Genetic disorder (e.g. hereditary angioedema), or other diseases.
Hives symptoms
Hives can change shape, move around, and may disappear only to reappear later. An interesting characteristic of hives is their ability to “blanch,” or turn white when pressed.
Like we mentioned before, there are two main types of hives – acute and chronic.
Acute hives are short-term, typically lasting less than six weeks, and are usually caused by an allergic reaction or infection.
Chronic hives, on the other hand, persist for more than six weeks and can be caused by various factors, often difficult to identify.
While hives are generally harmless and mostly cause discomfort, they can signal a serious allergic reaction if they appear in your throat and cause difficulty breathing. This should be treated as a medical emergency.
How long do hives last?
Hives that appear daily for longer than six weeks are called chronic hives, or chronic spontaneous urticaria.
Chronic hives resolve with over the counter treatments that include antihistamines, and anti-inflammatory medications or with more specialized treatment recommended by your allergy specialist.
Diagnosing hives
Hives may be in response to an allergic reaction or an autoimmune reaction. It is important to work with your allergy specialist to get a proper diagnosis. Hives should not be confused with the following conditions:
- Rashes are flat, can be blistering, flaking or cause broken skin.
- Bug bites do not move around and do not have multiple locations.
- Bed bug bites usually appear in a straight line and hives are usually more random in location.
- Angioedema causes swelling in the deeper layers of skin and under the fat.
- Vasculitis symptoms can include a non-blanching rash; the rash does not turn white when you press upon it.
- Contact dermatitis is your skin’s reaction to direct contact with an allergen.

How does AllerVie Health diagnose Hives?
Your AllerVie Health board-certified allergist will want to know if and when you have been exposed to something that may have triggered your hives. During your appointment they will review your medical history as well.
When to see a doctor about hives
If your hives don’t go away, you should make an appointment with a board-certified allergist. If you are having a serious allergic reaction that includes swelling under your skin or a life-threatening allergic reaction that includes trouble breathing, you should seek emergency care.
Make an Appointment
How does a doctor treat hives?
When it’s not possible to identify the trigger, your doctor may take one of several approaches to hives treatment.
Your doctor can recommend antihistamines that can ease symptoms to a degree or even stop hives from developing in the first place.
Patients with chronic hives may take antihistamines in tandem with other medications, including biologic drugs and steroids.
In the most severe cases, especially when severe angioedema occurs with hives, a patient may also require an injection of epinephrine or a steroid medication to immediately address swelling that affects respiratory pathways.
Patients can also undertake treatment for hives at home as a supplement to prescribed remedies.
Ways to treat hives at home
While you may see search results with varying recommendations for how to treat hives at home, it is recommended that you be seen by an allergist for this condition.
Tips to prevent hives breakouts
Here are some tips for preventing hives breakouts according to the American College of Allergy, Asthma & Immunology (ACAAI) and the American Academy of Allergy, Asthma & Immunology (AAAAI):
- Identify triggers: If you’ve had an outbreak of hives, try to identify what might have caused it. Keeping a diary of when the hives occur, what you were doing, eating, or exposed to could help identify patterns and potential triggers.
- Avoid known triggers: Once you’ve identified possible triggers, try to avoid them whenever possible. This may involve changes in diet, lifestyle, or the medications you take.
- Allergy testing: If you can’t identify a trigger, you may want to consider seeing an allergist for allergy testing. This can help identify if you’re allergic to specific substances.
- Stress management: Stress can sometimes trigger hives. Techniques for stress management, such as mindfulness, yoga, or regular exercise, can help.
- Medication: If your hives are recurrent and no specific trigger can be identified, or the trigger is unavoidable, your doctor may prescribe medication to help prevent them. Antihistamines are often used for this purpose.
- Avoid irritating your skin: Some people find that physical irritants, like tight clothing, can provoke hives. Wearing loose, comfortable clothes made of natural fibers can help.
- Maintain a healthy lifestyle: Regular exercise, a balanced diet, and adequate sleep can strengthen your immune system and make you less prone to allergic reactions.
Frequently asked questions
What’s the difference between hives and rashes?
Hives are all rashes, but not all rashes are hives. One distinguishing characteristic is that many rashes do not itch, while hives are always itchy. Hives also have very distinct bumps, whereas rashes can be scaly, flaky, or involve blisters. Rashes can also often feel very hot to the touch.
How long do hives last?
Hives can last an hour or two, or for as long as several weeks. Typically, hives caused from acute triggers, such as exposure to foods, resolve more quickly once the patient is no longer exposed to the trigger. Chronic cases lasting longer than six weeks may involve a secondary condition. In those scenarios, treating the other condition is an important part in resolving hives.
Can stress cause hives?
Yes, stress can cause hives. It is a common trigger of urticaria in adults. Stress hives are particularly common in women who are in their 30s, 40s, and 50s. Anyone experiencing hives from stress can reduce symptoms by treating the hives and addressing any stress triggers in their lives.
Are hives contagious?
Hives are not contagious. They are triggered by an immune response in the body and the release of histamines. You will not develop hives on your skin if you touch the affected skin of another person.
Why am I getting hives all of a sudden?
A variety of things can trigger hives; allergens, stress, even changes in temperature.
How do you get hives to go away?
If your hives last longer than 24 hours, you should consult an allergist.
